Dissecting bodies, exposing underlying illnesses, and treating patients are not the only activities conducted in the healthcare sector. Bills and payments are equally important but often problematic in healthcare organizations.
What is RCM software anyway, and how does it alleviate financial crises and setbacks in the healthcare department? In short, RCM software is the holy grail of healthcare finance management as it streamlines and automates administrative healthcare processes, especially those related to finance.
In this article, we’ll plunge into the nitty gritty of what RCM software is and the benefits that come with its incorporation. At the end of this article, you’ll deeply appreciate its role in the healthcare environment and its purpose.
Role of RCM Software in Healthcare
Firstly, we must address one essential and lingering question: what is RCM? Revenue Cycle Management (RCM) is a healthcare organization’s financial processes that cater to clinical operations and administrative procedures linked with revenue generation, claims processing, and payments.
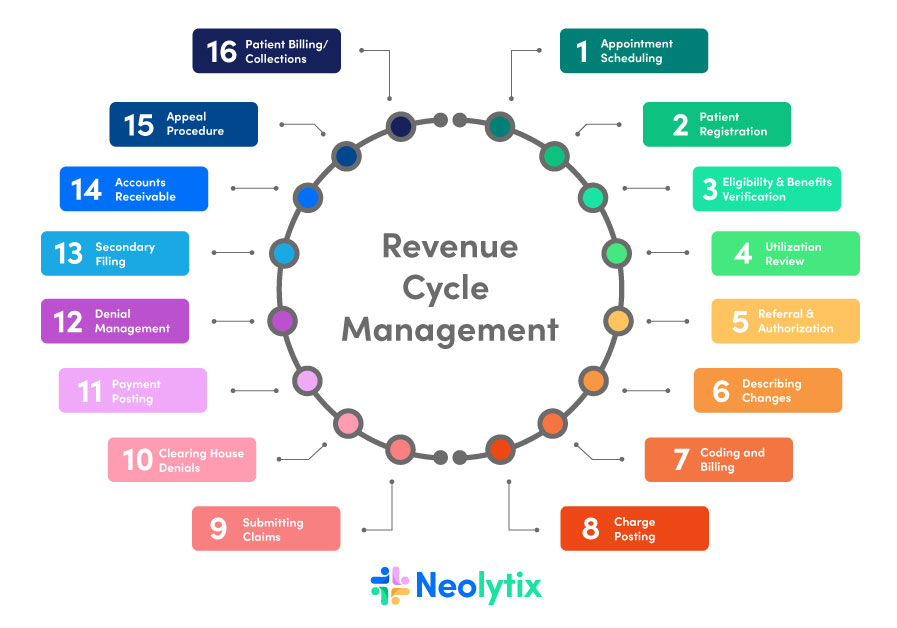
Then comes the second question: what is RCM software? It is a form of technology designed to automate and lighten the burden in the various components of the healthcare revenue cycle. Some of these components include:
- Insurance eligibility verification
- Appointment scheduling
- Patient registration and demographic information
- Claims submission
- Coding and billing
- Accounts and receivable management
- Reporting and analytics
- Payment posting
RCM software targets efficacy by reducing manual errors and enhancing the healthcare revenue cycle. It contributes to financial fitness by minimizing claim denials and accelerating payment cycles.
Whether deployed as a standalone or integrated with broader systems like the Healthcare Information System (HIS) or Electronic Health Record (EHR), its impact on revenue generation is significant.
Key Functions of RCM Software
RCM software activities involve key functions aimed at thoroughly handling the financial processes of healthcare organizations. These primary activities are explained below:
Patient Registration –
This function involves maintaining and capturing accurate patient demographic information. Documents must be scanned and analyzed to establish accurate billing, patient insurance plans, and coverage.
Appointment Scheduling –
To ensure seamless operations, prioritize setting proper schedules with the software. By avoiding overlaps and considering patient preferences, it establishes efficient appointment management.

Claims generation and submission –
Another critical function of the revenue cycle management software involves generating accurate, reliable, and complete claims for services rendered. These claims are shared with insurance service providers electronically or via other means available.
Coding and billing –
In this area, appropriate medical codes are assigned to services and procedures. Some of these medical codes include CPT and 1CD-10, to name a few. Bills for insurers and patients are rolled out according to benefits received.
Claim processing and adjudication –
The RCM management software monitors submitted claim statuses, handles claim denials, reviews appeals resubmissions, and ensures timely processing and payments.

Payment posting –
Record and reconciliation of payments from insurers and patients is conducted. After that, the system is updated with recent financial data. An updated system with accurate payment details irons out the possibility of overlooked dues or problems with already settled accounts.
Insurance eligibility and verification –
Patient insurance plans and coverage are scrutinized to determine patient benefits and limits.
Accounts receivable management –
In RCM management, records are exhumed. The software manages all unsettled dues and claims with patients, and the system establishes payment collection methods.
Reporting and Analytics –
For this task, the RCM software provides insight into the financial status and performance of the healthcare organization.

Reports are generated based on key metrics such as reimbursement rates, claims denials, and revenue accrued.
Advantages of RCM Software
Patient Registration and Instruction Verification –
The software guarantees faster and more accurate patient registration and billing procedures, inflating customer satisfaction.
Claims Processing and Management –
The RCM software provides optimized claims processing by monitoring claim statuses in real time. This results in reduced claim delays, denials, and enhanced reimbursement rates.
Payment Handling and Denial Management –
The RCM software manages outstanding balances and aging accounts. The system also carries the burden of follow-ups on unpaid claims and ultimately boosts collections.
Reporting for Financial Analysis –
More accurate and insightful reports are generated, giving a better understanding of KPIs that need to be honed and hammered for a better revenue cycle.

Selecting an Effective RCM System
Selecting an effective revenue cycle management system is a weighty process that carries great importance. It is crucial because it directly affects the financial wing and overall efficiency of healthcare organizations.
Some considerations can be put into practice to ensure the right RCM system is selected for the prosperity of healthcare finances.
Assess and Analyze Your Organization’s Needs
Fish out all loopholes and pain points in your organization’s revenue cycle. Brainstorm and finalize what features and operations best tackle the observed problems. Consider plans and methods that give room for scalability. It is futile to render myopic decision-making and disregard the future of the healthcare organization.
Define Clear Goals and Objectives
Draw out unequivocal objectives for the RCM system and software implementation process. Pinpoint and note KPIs the system should impact positively, such as improved billing accuracy.

Analyze Integration Capabilities
For whatever system has won your organization’s heart, ensure they seamlessly integrate with existing systems like electronic health records (EHR) and electronic medical records (EMR).
Security and Compliance
Every organization rests on specific regulations and laws. Make sure your selected RCM system complies with your healthcare organization’s regulations. One regulatory board to verify with is HIPAA. Analyze and assess the system’s security measures to safeguard patient-sensitive information.
User-Friendly and Flexible System
Aim for a user-friendly and easy-to-integrate system to reduce or eliminate staff members’ resistance. Consider giving your staff training for a smooth transition into the newly elected RCM management system.

A more flexible approach will yield better adaptability to your organization’s healthcare policies and regulations.
Consider Vendor Reputation and Support
Initiate your RCM management system search by researching and listing potential vendors. Scrutinize client histories, reviews, and ratings to gauge their reputation. Evaluate the level of support each vendor offers. Inquire about training and implementation benefits to ensure a seamless transition into your new system.
Cost Considerations
When adopting a new RCM management system, carefully assess all associated costs. Consider upfront expenses, ongoing maintenance costs, licensing fees, and additional short and long-term expenditures to ensure a comprehensive understanding of ownership expenses.
Data Analytics and Reports
Check your system’s ability to generate meaningful reports and analytics data. The generated reports should give a proper glimpse of the organization’s financial performance.

A poor analytics system means shooting your healthcare organization in the foot.
See Also: 5 Best Article Submission Software in 2024
Performance and Reliability
Once you’ve selected a new system, assess its reliability and performance. Evaluate its alignment with existing workflows, ensuring it streamlines irregularities. Inquire about the vendor’s damage and disaster recovery plan for added assurance.
See Also: 8 Best Graphic Design Software Free Download
Trial and Demonstration
Before committing to an RCM management system, request a trial period. Engage with the vendor, seeking a demonstration that showcases its functionality in real-life situations.
See Also: 10 Best Clothing Design Software To Download for Mac
FAQs
What are the four major components of RCM?
The four major components of RCM include proactive, reactive, condition, and time-based tasks.
What are the duties of an RCM?
The duties or tasks involved in RCM vary depending on the role assigned within the healthcare system. Tasks include but are not limited to patient registration, appointment scheduling, payment collections, and insurance verifications.
What is the highest salary in RCM?
The salaries depend on the individual’s experience, size of the organization, location of the organization, etc. The highest recorded annual salary is as an RCM manager or director with a lucrative $100,000 tag.
Is RCM a good industry?
According to employee responses, the RCM industry is perfect, with an impressive 4.2 rating. Unlike other sectors where job security is unstable, the industry scores a 4.3 on the rating index, which is very positive.
What is the salary of an RCM software engineer?
In the United States, the starting salary at the entry-level may range between $60 000 and $80 000, with mid-level wages between $80 000 and $100 000. Senior level can earn anywhere between $100 000 and $130 000. The salaries vary with location and the region's economic situation or country of residence.
Conclusion
The creation of RCM software aims to introduce optimized finance handling procedures. Moreover, it seeks to eradicate errors and streamline hefty tasks in RCM management.
A well-implemented RCM software and system yield optimistic future projections for the healthcare system’s financial fitness. Explore the transformative realm of RCM software in our article. Uncover its benefits and witness significant yet beneficial changes upon implementation in your healthcare organization.
See Also: 10 Best Free & Paid Flowchart Software | Windows & Mac
Mitchel Broussard: Deals Editor at MacRumors since 2014. Oversees daily deals coverage, writes articles, updates guides, manages partnerships, and more.